22/09/2013
Pansement hémostatique:Vraiment utile ?
Watters J et all. J Trauma. 2011;70:1413–1419
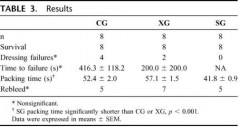
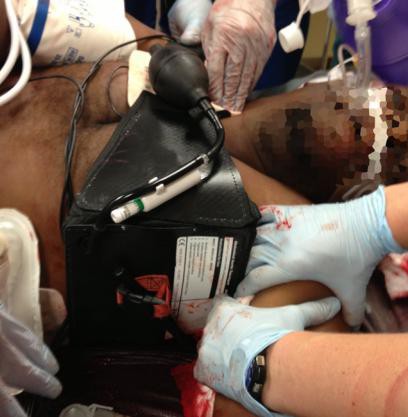
Un travail intéressant qui s'interroge sur le vrai intérêt des pansements hémostatiques. Sans remettre en question ce dernier cet article remet en question le positionnement de ce type de matériel. Dans un travail expérimental sur un modèle animal, un packing de plaie avec de la gaze simple serait plus rapide et tout aussi efficace qu'un packing effectué avec le Combat gauze ou le celox gauze.
-----------------------------------------------------------------
Results: All animals survived to study end. There were no differences in baseline physiologic or coagulation parameters or in dressing success rate (SG: 8/8, CG: 4/8, XG: 6/8) or blood loss between groups (SG: 260 mL, CG: 374 mL, XG: 204 mL; p > 0.3). SG (40 seconds ± 0.9 seconds) packed significantly faster than either the CG (52 ± 2.0) or XG (59 ± 1.9). At 120 minutes, all groups had a significantly shorter time to clot formation compared with baseline (p < 0.01). At 30 minutes, the XG animals had shorter time to clot compared with SG and CG animals (p < 0.05). All histology sections had mild intimal and medial edema. No inflammation, necrosis, or deposition of dressing particles in vessel walls was observed. No histologic or ultrastructural differences were found between the study dressings.
-----------------------------------------------------------------
"There are reasons that standard woven gauze bandages have existed for millennia. They are lightweight, absorbent, highly conformable, stable in a variety of environmental conditions, and inexpensive. Multiple advanced hemostatic agents have resulted in superior homeostasis, improved outcomes, and likely saved lives compared with SG when applied according to manufacturers’ recommendations for compression time. However, in a care under fire scenario or in a situation of mass casualties, compression times of 2 minutes to 5 minutes are not feasible. During ongoing battle, only lifethreatening injuries should be addressed and often the wounded must self-apply a tourniquet or dressing. An individual rendering self or buddy aid will need to continue to engage in battle as the first priority. Major vascular injuries, which cannot be controlled through application of a tourniquet, must be addressed as quickly as possible before profound bleeding incapacitates the casualty. Similarly, when there are persons with multiple injuries or wounds to treat, dressings must be rapidly placed and effective without prolonged hold times"
Conclusion: Ce qui compte c'est la compression et le packing de plaie
| Tags : pansement
SFMU
SFAR - Recommandations
Crush Syndrome et rhabdomyolyse
| Tags : crush
Recommendations for the Management of Crush Victims in Mass Disasters
| Tags : crush
Rhabdomyolyse – Crush syndrome
Rhabdomyolyse – Crush syndrome
Mis en ligne le 22 Juillet 2013 Imprimer cette page

Dr Ségolène MROZEK, Pr Thomas GEERAERTS
Pôle Anesthésie-Réanimation, CHU de Toulouse
Question 1
La valeur de créatinine phosphokinase (CPK) prédit-elle le développement d’une insuffisance rénale aigue lors d’une rhabdomyolyse ?
La nécrose musculaire conduit à la libération du contenu cellulaire et notamment des enzymes impliquées dans le fonctionnement musculaires comme la créatinine phosphokinase (CPK). La rhabdomyolyse est définie par une élévation de la concentration plasmatique des CPK à plus de 5 fois la normale (soit environ 1000 UI/L) dont le pic est tardif (24 à 36 heures) [1]. La demi-vie plasmatique des CPK chez les patients présentant une rhabdomyolyse est de l’ordre de 42 heures [2].
Brown et al. ont relevé, parmi 2083 patients traumatisés, une rhabdomyolyse dans 85% des cas. Dix pour cent des patients développaient une insuffisance rénale aiguë (créatinine > 2 mg/dl) et 5 % nécessitaient le recours à la dialyse. Une concentration plasmatique de CPK > 5 000 UI/L était un facteur de risque indépendant d’insuffisance rénale aigue (IRA) [3]. Ce seuil de 5 000 UI/L est confirmé la même année par une autre équipe chez 148 patients [4]. Un modèle prédisant la survenue d’insuffisance rénale aiguë (IRA) lors d’une rhabdomyolyse développé par Ward et al. en 1988 avait par ailleurs retenu : les valeurs plasmatiques de CPK, du potassium, du phosphore, de l’albumine, la présence d’une déshydratation à la prise en charge du patient et la survenue d’un sepsis pendant le séjour [5]. Plus récemment, El-Abdellati et al. [6] rapportent chez 342 patients présentant une rhabdomyolyse à l’admission en réanimation, une association entre la valeur des CPK plasmatiques (surtout pour CPK> 5 000 UI/L), et la sévérité des défaillances d’organe (score SOFA), la survenue d’une IRA (risque x5) ainsi que le pronostic. Les auteurs soulignent lors de leur analyse par régression logistique que même des valeurs de CPK > 1000 UI/L étaient associées à une augmentation significative du risque de développement d’IRA (augmentation du risque par 3). En accord avec ces données, les sociétés savantes recommandent une surveillance accrue de la fonction rénale chez les patients présentant un taux de créatinine > 150 μmol/L et/ou des CPK > 5000 UI/L devant le risque accru d’IRA [7].
Des études récentes suggèrent que la myoglobine plasmatique et urinaire serait un meilleur marqueur prédictif d’IRA lors de rhabdomyolyse compte tenu de sa cinétique plus précoce [6, 8].
Question 2
Doit-on administrer des solutés contenant des bicarbonates lors d’une rhabdomyolyse ?
Le pH urinaire influence la précipitation de la myoglobine dans les tubules rénaux et est donc l’un des principaux déterminant de survenue d’insuffisance rénale aiguë [9]. Soixante-treize pourcents de la myoglobine urinaire précipitent si le pH urinaire est inférieur à 5. A l’opposé, seul 4 % de la myoglobine précipite à pH 6,5 [10]. L’alcalinisation des urines et l’obtention d’une diurèse importante (effet de lavage et de dilution tubulaire de la myoglobine) sont donc primordiaux jusqu’à la disparition de la myoglobinurie (soit habituellement en 72 heures).
La volémie plasmatique influence le pH urinaire. Si on se réfère aux phénomènes d’acidurie engendrés par l’hyperaldostéronisme secondaire dû à l’hypovolémie, l’expansion volémique à elle seule pourrait suffire à atteindre les objectifs de diurèse et d’alcalinisation des urines [11, 12]. Un remplissage vasculaire « optimal » pourrait alors être guidé par l’évolution du pH urinaire et de la diurèse. Un objectif thérapeutique raisonnable pourrait être l’obtention d’un pH urinaire supérieur ou égal à 6,5 à la bandelette urinaire.
Cependant, certains auteurs recommandent la perfusion de bicarbonates afin d’alcaliniser les urines en complément du remplissage vasculaire [13,14]. La perfusion de bicarbonates entraîne une augmentation du pH sanguin suivie, en l’absence d’hypovolémie, d’une augmentation du pH urinaire. L’alcalose ainsi créée peut toutefois contribuer à la précipitation du calcium dans les tissus mous et aggraver l’hypocalcémie existante. Dans cette situation rare (pH sang > 7,5), l’administration d’acétazolamide (Diamox®) permettrait de limiter ces dépôts phosphocalciques [11]. La littérature n’a pas montré de réel bénéfice à l’administration de bicarbonates de sodium comparé aux cristalloïdes dans la fréquence de survenue d’IRA ou le recours à la dialyse lors de rhabdomyolyse [3,7]. Néanmoins, l’administration massive de sérum salé isotonique peut contribuer à une acidose métabolique hyperchlorémique. Ainsi, certaines équipes ont montré que le maintien d’un pH urinaire > 6,5 uniquement avec un remplissage par sérum salé isotonique était difficile à obtenir [15, 16]. Malgré une littérature controversée, l’administration combinée de bicarbonates de sodium et de sérum salé isotonique est utilisée par certains après la restauration initiale de la volémie lorsque le pH urinaire reste inférieur à 6,5 [17]. Ceci suppose de surveiller le pH urinaire, la concentration plasmatique de bicarbonate, la calcémie et la kaliémie. En l’absence d’augmentation du pH urinaire 4 à 6 heures après la perfusion de bicarbonates et si des symptômes d’hypocalcémie apparaissent, l’alcalinisation est arrêtée. Plus simplement, une étude récente a montré qu’un remplissage vasculaire par du Ringer Lactate permettait d’obtenir assez facilement une alcalinisation des urines, sans recours aux bicarbonates et sans induire d’acidose métabolique ni d’hyperkaliémie [16]. Ainsi, plus que l’alcalinisation du plasma par l’administration de bicarbonate, c’est bien la correction d’une hypovolémie avec un ou des solutés adaptés qui semble à privilégier pour prévenir la précipitation de la myoglobine urinaire.
Question 3
Doit-on effectuer une diurèse forcée par des diurétiques lors d’une rhabdomyolyse ?
L’objectif consensuel pour la prise en charge de la rhabdomyolyse est d’obtenir une diurèse > 2 à 3 ml/kg/h grâce au remplissage vasculaire. Après s’être assuré d’une volémie suffisante, la clairance rénale de la myoglobine pourrait être améliorée grâce à une diurèse forcée mais son utilisation reste controversée [2]. Cette diurèse peut être obtenue par l’utilisation des diurétiques classiques ou par diurèse osmotique (mannitol).
Au niveau rénal, le mannitol pourrait avoir plusieurs effets bénéfiques : une vasodilatation, une augmentation de la pression tubulaire et une augmentation de la filtration glomérulaire [18]. Le mannitol possède également un pouvoir antioxydant. De par son pouvoir osmotique, il permet également de diminuer la pression au niveau des loges musculaires lésées, et en théorie de diminuer l’œdème musculaire. L’utilisation du mannitol est toutefois controversée. Son utilisation ne semble pas produire des résultats supérieurs à l’expansion volémique seule [12], et son utilisation pourrait même être dangereuse pour le rein en cas d’hypovolémie induite par ses effets diurétiques puissants difficilement contrôlables [19]. La diurèse induite par le mannitol, si elle est utilisée, devra donc être compensée. Les recommandations de 2012 dans la prise en charge des patients victimes d’un crush syndrome ne retiennent pas de preuve de son efficacité [20].
L’emploi des diurétiques de l’anse pourrait être également possible chez les sujets dont la diurèse est insuffisante. Cependant, le furosémide entraîne une acidification des urines potentiellement délétère, une alcalinisation sanguine ainsi qu’une perte calcique urinaire pouvant aggraver l’hypocalcémie préexistante. Les diurétiques de l’anse, en inhibant la réabsorption du sodium, permettent expérimentalement une amélioration de l’oxygénation de la médullaire rénale grâce à une « mise au repos » de ces structures [21]. Ces effets sont en théorie intéressants afin de réduire le stress ischémique tubulaire. Le bénéfice des diurétiques n’a cependant pas été confirmé par des études cliniques dans la rhabdomyolyse. Les diurétiques doivent être utilisés avec précaution et uniquement après correction d’une hypovolémie [7,17]. Dans le cadre d’une diurèse forcée par diurétiques de l’anse, l’utilisation simultanée d’acétazolamide (Diamox®) permettrait grâce à une élimination urinaire de bicarbonates de respecter les valeurs de pH urinaires recherchées.
L’usage des diurétiques reste donc délicat et son bénéfice clinique est encore à démontrer.
Question 4
Quelle quantité de fluides doit-on administrer lors de la prise en charge initiale d’un patient présentant un crush syndrome ?
Pour corriger l’hypovolémie majeure présente initialement, la perfusion de large volume de solutés est indispensable en limitant en première intention les apports de solutions contenant des quantité importantes de potassium [20]. Le remplissage vasculaire doit être précoce afin de diminuer les risques de survenue d’une IRA et doit commencer dès la phase pré-hospitalière. Better et al. en 1990 ont proposé un protocole de remplissage vasculaire pour la prise en charge des patients victimes d’un tremblement de terre [13]. Il convient de noter que dans cette publication princeps, le protocole n’a pas été établi à partir de données cliniques, mais de façon empirique sans réelle validation. Dans ce protocole, 1 L de sérum salé isotonique par heure était administré sur place puis après évacuation 2 à 3 L de sérum salé 4,5%+ bicarbonates de sodium 50 mEq pour un objectif de pH urinaire > 6,5. Si une oligurie persistait, les patients recevaient alors 50 mL de mannitol 20%. Des volumes supérieurs à une dizaine de litres par jour (12 L/24h) pendant 48 à 72 heures étaient nécessaires, au prix d’une rétention hydrosodée conséquente. Il semblerait que son application aux victimes de tremblement de terre permette d’éviter l’apparition de l’insuffisance rénale et d’obtenir une survie optimale [22]. Guna et al. ont utilisé ce même protocole chez 16 patients présentant un crush syndrome lors d’un séisme en Turquie. Les victimes recevaient en moyenne 20 L/jour. Cette charge hydrosodée était bien tolérée probablement en raison du jeune âge des patients (âge moyen : 23 ans). De tels volumes de remplissage vasculaire sont cependant à considérer du fait du risque d’aggravation des fréquents syndromes de détresse respiratoire aiguë (SDRA) observés au décours des rhabdomyolyses majeures [23]. L’impact pronostique du SDRA restant plus délétère que celui d’une IRA liée à une rhabdomyolyse, même anurique, susceptible de récupérer après 3 semaines de dialyse. Une attention particulière doit être donnée à la fonction pulmonaire en prenant en compte la balance bénéfice/risque du remplissage. Devant un pH urinaire alcalin (pH > 6) et en l’absence de myoglobinurie à la bandelette, le remplissage vasculaire devra être freiné.
Ainsi nous pouvons proposer, selon les recommandations de 2012 pour les patients victimes d’un crush syndrome [20] : une initiation rapide, la plus précoce possible, d’un remplissage vasculaire par du sérum salé isotonique à un débit initial de 1000 mL/ h. Les patients devront être réévalués toutes les 6 heures et le remplissage devra être individualisé pour chaque patient par un monitorage hémodynamique adapté (échocardiographie par exemple). Il faut alors tenir compte de ses antécédents notamment cardiorespiratoires, son âge et évaluer son état hémodynamique ainsi que sa diurèse. L’objectif est donc une diurèse de 2 à 3 ml/h avec un pH urinaire > 6,5. Le monitorage hémodynamique sera primordial par la suite pour adapter au mieux le remplissage vasculaire avec une surveillance stricte de la fonction pulmonaire. En l’absence de monitorage possible, la quantité de fluide pourra être d’environ 3 à 6 L/24H.
REFERENCES
[9] Zager RA. Rhabdomyolysis and myohemoglobinuric acute renal failure. Kidney Int 1996; 49: 314-326.
[10] Gonzalez D. Crush syndrome. Crit Care Med 2005; 33: S34-41.
[17] Bosch X, Poch E, Grau JM. Rhabdomyolysis and acute kidney injury. N Engl J Med 2009; 361: 62-72.
| Tags : crush
21/09/2013
Contamination des plaies: A l'entrée et la sortie
Effect of Initial Projectile Speed on Contamination Distribution in a Lower Extremity Surrogate “Wound Track”
Krebsbach MA et All., Military Medicine, 177, 5:573, 2012
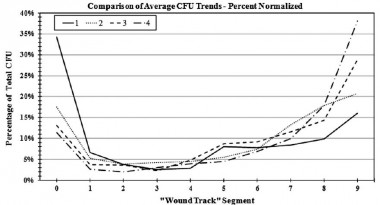
Le nettoyage précoce et la couverture des orifices d'entrée et de sortie sont donc théoriquement des maillons importants de la lutte contre l'infection des plaies de guerre.
| Tags : infection, balistique, pansement
Chemical Terrorism for the Intensivist
Chemical Terrorism for the Intensivist
Chalela J et All. Military Medecine, 177, 5:495, 2012
The use of chemical agents for terrorist attacks or military warfare is a major concern at the presenttime. Chemical agents can cause significant morbidity, are relatively inexpensive, and are easy to store and use.Weaponization of chemical agents is only limited by the physicochemical properties of some agents. Recent incidentsinvolving toxic industrial chemicals and chemical terrorist attacks indicate that critical care services are frequentlyutilized. For obvious reasons, the critical care literature on chemical terrorism is scarce. This article reviews the clinicalaspects of diagnosing and treating victims of chemical terrorism while emphasizing the critical care management. Theintensivist needs to be familiar with the chemical agents that could be used in a terrorist attack. The military classification divides agents into lung agents, blood agents, vesicants, and nerve agents. Supportive critical care is the cornerstoneof treatment for most casualties, and dramatic recovery can occur in many cases. Specific antidotes are available forsome agents, but even without the antidote, aggressive intensive care support can lead to favorable outcome in manycases. Critical care and emergency services can be overwhelmed by a terrorist attack as many exposed but not ill willseek care.
| Tags : nrbc
19/09/2013
Causes et lieux de décès au combat: Actualisation
Death on the battlefield (2001-2011): Implications for the future of combat casualty care.
Eastdrige BJ et All. , J Trauma Acute Care Surg. 2012;73: S431-S437
Une publication n'est pas récente mais qui a pour intérêt d'actualiser la question à l'aulne de la dizaine d'années de combats asymétriques en afghanistan et en irak.
BACKGROUND: Critical evaluation of all aspects of combat casualty care, including mortality, with a special focus on the incidence and causes of potentially preventable deaths among US combat fatalities, is central to identifying gaps in knowledge, training, equipment, and execution of battlefield trauma care. The impetus to produce this analysis was to develop a comprehensive perspective of battlefield death, concentrating on deaths that occurred in the preYmedical treatment facility (pre-MTF) environment.
METHODS: The Armed Forces Medical Examiner Service Mortality Surveillance Division was used to identify Operation Iraqi Freedom and operation Enduring Freedom combat casualties from October 2001 to June 2011 who died from injury in the deployed environment.bThe autopsy records, perimortem records, photographs on file, and Mortality Trauma Registry of the Armed Forces Medical Examiner Service were used to compile mechanism of injury, cause of injury, medical intervention performed, Abbreviated Injury Scale (AIS)score, and Injury Severity Score (ISS) on all lethal injuries. All data were used by the expert panel for the conduct of the potential for injury survivability assessment of this study.
RESULTS: For the study interval between October 2001 and June 2011, 4,596 battlefield fatalities were reviewed and analyzed. The stratificationof mortality demonstrated that 87.3% of all injury mortality occurred in the pre-MTF environment. Of the pre-MTF deaths, 75.7%(n = 3,040) were classified as nonsurvivable, and 24.3% (n = 976) were deemed potentially survivable (PS). The injury/physiologic focus of PS acute mortality was largely associated with hemorrhage (90.9%). The site of lethal hemorrhage was truncal (67.3%), followed by junctional (19.2%) and peripheral-extremity (13.5%) hemorrhage.
CONCLUSION: Most battlefield casualties died of their injuries before ever reaching a surgeon. As most pre-MTF deaths are nonsurvivable, mitigation strategies to impact outcomes in this population need to be directed toward injury prevention. To significantly impact the outcome of combat casualties with PS injury, strategies must be developed to mitigate hemorrhage and optimize airway management or reduce the time interval between the battlefield point of injury and surgical intervention. Understanding battlefield mortality is a vital component of the military trauma system. Emphasis on this analysis should be placed on trauma system optimization, evidence-based improvements in Tactical Combat Casualty Care guidelines, data-driven research, and development to remediate gaps in care and relevant training and equipment enhancements that will increase the survivability of the fighting force.
14/09/2013
Réalité augmentée et sauvetage au combat: Bientôt ?
Using augmented reality as a clinical support tool to assist combat medics in the treatment of tension pneumothoraces.
Wilson KL et All. Mil Med 2013; 178(9):981-5
----------------------------------------------------------------------------------------
La réalité augmentée désigne les systèmes informatiques qui rendent possible la superposition d'un modèle virtuel 3D ou 2D à la perception que nous avons naturellement de la réalité et ceci en temps réel. La commercialisation récente des Google glass est le témoin d'une technologie qui devient mature. Dès lors il n'est pas étonnant qu'un tel dispositif soit utilisé dans les domaines de la formation voire en conditions réelles. Le travail présenté ci-après n'est qu'un exemple.
----------------------------------------------------------------------------------------
This study was to extrapolate potential roles of augmented reality goggles as a clinical support tool assisting in the reduction of preventable causes of death on the battlefield. Our pilot study was designed to improve medic performance in accurately placing a large bore catheter to release tension pneumothorax (prehospital setting) while using augmented reality goggles. Thirty-four preclinical medical students recruited from Morehouse School of Medicine performed needle decompressions on human cadaver models after hearing a brief training lecture on tension pneumothorax management. Clinical vignettes identifying cadavers as having life-threatening tension pneumothoraces as a consequence of improvised explosive device attacks were used. Study group (n = 13) performed needle decompression using augmented reality goggles whereas the control group (n = 21) relied solely on memory from the lecture. The two groups were compared according to their ability to accurately complete the steps required to decompress a tension pneumothorax. The medical students using augmented reality goggle support were able to treat the tension pneumothorax on the human cadaver models more accurately than the students relying on their memory (p < 0.008). Although the augmented reality group required more time to complete the needle decompression intervention (p = 0.0684), this did not reach statistical significance.
| Tags : pédagogie, simulateurs
13/09/2013
Physical fitness: Une nécessité ?
Psychological Health and Traumatic Brain Injury
08/09/2013
Stabilisation pelvienne: Vraiment utile !
Emergency stabilization of the pelvic ring: Clinical comparison between three different techniques
Pizanis A. et All. Injury. 2013 Aug 2. pii: S0020-1383(13)00316-1.
Background: Emergency devices for pelvic ring stabilization include circumferential sheets, pelvic binders, and c-clamps. Our knowledge ofthe outcome ofthese techniques is currently based on limited information.
Methods: Using the dataset of the German Pelvic Trauma Registry, demographic and injury-associated characteristics as well as the outcome of pelvic fracture patients after sheet, binder, and c-clamp treatment was compared. Outcome parameters included transfusion requirement of packed red blood cells, length of hospital stay, mortality, and incidence of lethal pelvic bleeding.
Results: Two hundred seven of 6137 (3.4%) patients documented in the German Pelvic Trauma Registry between April 30th 2004 and January 19th 2012 were treated by sheets, binders, or c-clamps. In most cases, c-clamps (69%) were used, followed by sheets (16%), and binders (15%). The median age was significantly lower in patients treated with binders than in patients treated with sheets or c-clamps (26 vs. 47 vs. 42 years, p = 0.01). Sheet wrapping was associated with a significantly higher incidence of lethal pelvic bleeding compared to binder or c-clamp stabilization (23% vs. 4% vs. 8%). No significant differences between the study groups were found in sex, fracture type, blood haemoglobin concentration, arterial blood pressure, Injury Severity Score, the incidence of additional pelvic packing and arterial embolization, need of red blood cell transfusion, length of hospitalisation, and mortality.
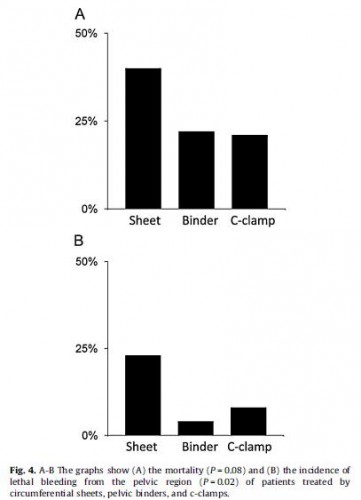
Conclusions: The data suggest that emergency stabilization ofthe pelvic ring by binders and c-clamps is associated with a lower incidence of lethal pelvic bleeding compared to sheet wrapping.
| Tags : pelvis
07/09/2013
Blast des membres
Blast-related fracture patterns: a forensic biomechanical approach
Ramasamy A. et All. J. R. Soc. Interface (2011) 8, 689–698
Dehors et dedans, ce n'est pas la même chose
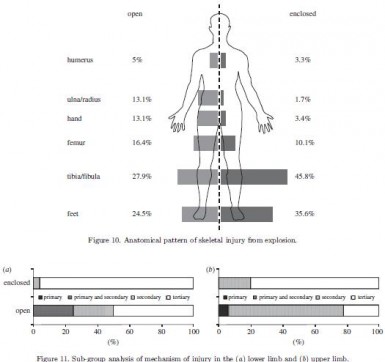
Les lésions dépendent du type de blast
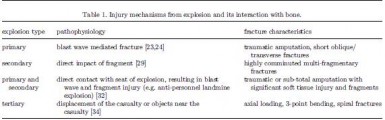

| Tags : blast
La cheville et le pied: C'est grave AUSSI
Outcomes of IED Foot and Ankle Blast Injuries
Ramasamy A et All. J Bone Joint Surg Am. 2013;95:e25(1-7)
Background: Improvements in protection and medical treatments have resulted in increasing numbers of modernwarfare casualties surviving with complex lower-extremity injuries. To our knowledge, there has been no prior analysis of foot and ankle blast injuries as a result of improvised explosive devices (IEDs). The aims of this study were to report the pattern of injury and determine which factors are associated with a poor clinical outcome.
Methods: U.K. service personnel who had sustained lower leg injuries following an under-vehicle explosion from January 2006 to December 2008 were identified with the use of a prospective trauma registry. Patient demographics, injury severity, the nature of the lower leg injury, and the type of clinical management were recorded. Clinical end points were determined by (1) the need for amputation and (2) ongoing clinical symptoms.
Results: Sixty-three U.K. service personnel (eighty-nine injured limbs) with lower leg injuries from an explosion were identified. Fifty-one percent of the casualties sustained multisegmental injuries to the foot and ankle. Twenty-six legs (29%) required amputation, with six of them amputated because of chronic pain eighteen months following injury. Regression analysis revealed that hindfoot injuries, open fractures, and vascular injuries were independent predictors ofamputation. At the time of final follow-up, sixty-six (74%) of the injured limbs had persisting symptoms related to the injury,and only nine (14%) of the service members were fit to return to their preinjury duties.
Conclusions: This study demonstrates that foot and ankle injuries from IEDs are associated with a high amputation rateand frequently with a poor clinical outcome. Although not life-threatening, they remain a source of long-term morbidity in an active population
On insiste beaucoup sur la gravité des lésions des membres inférieurs car elles sont sources d'hémorragies graves. Cette gravité est aussi fonctionnelle. Les auteurs de ce document insistent sur la fréquence de l'atteinte de la cheville et du pied (plus d'une fois sur 2), sur la gravité de l'atteinte de la cheville et de l'arrière pied et de la fréquence des amputations près d'une fois sur 3
Causes de DC évitables: Actualisation UK
Identifying future ‘unexpected’ survivors: a retrospective cohort study of fatal injury patterns in victims of improvised explosive devices
To identify potentially fatal injury patterns in explosive blast fatalities in order to focus research and mitigation strategies, to further improve survival rates from blast trauma.
DESIGN:
Retrospective cohort study.
PARTICIPANTS:
UK military personnel killed by improvised explosive device (IED) blasts in Afghanistan, November 2007-August 2010.
SETTING:
UK military deployment, through NATO, in support of the International Security Assistance Force (ISAF) mission in Afghanistan.
DATA SOURCES:
UK military postmortem CT records, UK Joint Theatre Trauma Registry and associated incident data.
MAIN OUTCOME MEASURES:
Potentially fatal injuries attributable to IEDs.
RESULTS:
We identified 121 cases, 42 mounted (in-vehicle) and 79 dismounted (on foot), at a point of wounding. There were 354 potentially fatalinjuries in total. Leading causes of death were traumatic brain injury (50%, 62/124 fatal injuries), followed by intracavity haemorrhage (20.2%, 25/124) in the mounted group, and extremity haemorrhage (42.6%, 98/230 fatal injuries), junctional haemorrhage (22.2%, 51/230 fatal injuries) and traumatic brain injury (18.7%, 43/230 fatal injuries) in the dismounted group.
CONCLUSIONS:
Head trauma severity in both mounted and dismounted IED fatalities indicated prevention and mitigation as the most effective strategies to decrease resultant mortality. Two-thirds of dismounted fatalities had haemorrhage implicated as a cause of death that may have been anatomically amenable to prehospital intervention. One-fifth of the mounted fatalities had haemorrhagic trauma which currently could only be addressed surgically. Maintaining the drive to improve all haemostatic techniques for blast casualties, from point of wounding to definitive surgical proximal vascular control, alongside the development and application of novel haemostatic interventions could yield a significant survival benefit. Prospective studies in this field are indicated.
Cette publication est très importante car elle insiste sur l'absolue nécessité de poursuivre les efforts en vue de prévenir le trauma aussi bien en matière de protection balistique, de réduction des délais de transports pour permettre la prise en charge d'hémorragie intra-cavitaires et l'aspect fondamental d'arrêter toutes les hémorragies sur le terrain notamment pas la mise en oeuvre d'une nouvelle catégorie de garrots pour les hémorragies jonctionnelles (voir 1, 2, 3, 4, 5, 6)
Les morts par IED sont plus sévèrement atteints dans un véhicule qu'à pied.
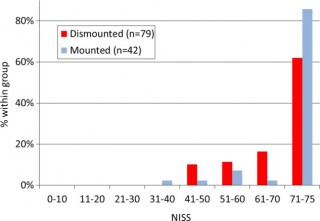
58% des Décès sont liés à plus de 2 causes potentiellement évitables
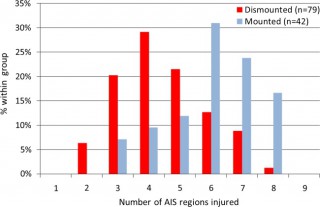
Les causes de décès ne sont pas les mêmes en combat à pied ou en véhicule
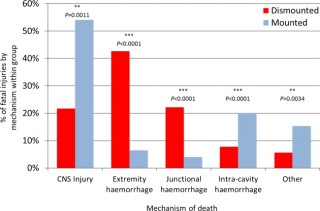
| Tags : balistique, blast, traumatologie, explosion, jonctionnel
06/09/2013
Tourniquet abdominal: Compression axillaire ?
| Tags : tourniquet, hémorragie, jonctionnel
04/09/2013
Prévention du suicide dans les armées
| Tags : psychiatrie, suicide
Chemical and biological weapons
Fiches Biotox
Fiches biotox de prise en charge thérapeutique
Ces fiches sont destinées aux professionnels de santé habilités à appliquer les instructions du plan BIOTOX.
- Introduction aux fiches biotox de prise en charge thérapeutique (24/10/2008)
- Fiche récapitulative (24/10/2008)
- Conduite à tenir en situation d'urgence avant identification de l'agent pathogène responsable (24/10/2008)
- Vademecum thérapeutique (24/10/2008)
- Indications et alternatives thérapeutiques aux fluoroquinolones (24/10/2008)
- Fiche 2 - Charbon (24/10/2008)
- Fiche 3 - Peste (24/10/2008)
- Fiche 4 -Tularémie (23/10/2008)
- Fiche 5 - Brucellose (24/10/2008)
- Fiche 6 - Agents des fièvres hémorragiques virales (24/10/2008)
- Fiche 7 - Variole (24/10/2008)
- Fiche 8 - Toxine botulique (24/10/2008)
- Fiche 9 - Fièvre Q (24/10/2008)
- Fiche 10 - Morve et mélioïdose (24/10/2008)
- Fiche 11 - Autres infections bactériennes (24/10/2008)
- Fiche 12 - Autres agents biologiques, pour lesquels aucun traitements spécifique ou prophylactique ne peut être recommandés (24/10/2008)