30/04/2012
Sédation dissociative: La Kétamine
| Tags : kétamine
Recours à la morphine et PTSD
Morphine Use after Combat Injury in Iraq and Post-Traumatic Stress Disorder.
Holbrook TL et all. N Engl J Med 2010;362:110-7.
Background
Post-traumatic stress disorder (PTSD) is a common adverse mental health outcome among seriously injured civilians and military personnel who are survivors of trauma. Pharmacotherapy in the aftermath of serious physical injury or exposure to traumatic events may be effective for the secondary prevention of PTSD.
Methods
We identified 696 injured U.S. military personnel without serious traumatic brain injury from the Navy–Marine Corps Combat Trauma Registry Expeditionary Medical Encounter Database. Complete data on medications administered were available for all personnel selected. The diagnosis of PTSD was obtained from the Career History Archival Medical and Personnel System and verified in a review of medical records.
Results
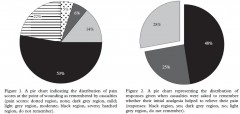
Among the 696 patients studied, 243 received a diagnosis of PTSD and 453 did not. The use of morphine during early resuscitation and trauma care was significantly associated with a lower risk of PTSD after injury. Among the patients in whom PTSD developed, 61% received morphine; among those in whom PTSD did not develop, 76% received morphine (odds ratio, 0.47; P<0.001). This association remained significant after adjustment for injury severity, age, mechanism of injury, status with respect to amputation, and selected injury-related clinical factors.
Conclusions
Our findings suggest that the use of morphine during trauma care may reduce the risk of subsequent development of PTSD after serious injury.
28/04/2012
La douleur du blessé de guerre: La vision UK
The injured mind in the UK Armed Forces
The mental health of the UK Armed Forces is a topic much debated by healthcare professionals, politicians and the media.While the current operations in Afghanistan, and the recent conflict in Iraq, are relevant to this debate, much of what is known about the effects of war upon the psyche still derives from the two World Wars. This paper will examine the historical and contemporary evidence about why it is that some Service personnel suffer psychological injuries during their military service and others do not. The paper will also consider some of the strategies that today’s Armed Forces have put in place to mitigate the effects of sending military personnel into danger.
http://rstb.royalsocietypublishing.org/content/366/1562/2...
| Tags : psychiatrie, ptsd
Guide pédagogique du sauvetage au combat 2012
50 batailles qui ont changé le monde
22/04/2012
Use of tourniquets and their effects on limb function in the modern combat environment
Use of tourniquets and their effects on limb function in the modern combat environment
Kragh JF Foot Ankle Clin N Am 15 (2010) 23–40
Un article à lire avec attention car il exprime bien à la fois l'histoire des garrots et les enjeux actuels
| Tags : tourniquet
20/04/2012
Brancard d'exctraction: Emploi d'un filet anti-châleur
| Tags : brancardage
18/04/2012
Conférence Experts: Intubation difficile
| Tags : intubation
Médecine de montagne
| Tags : montagne
Manuel de survie US
Medical Aspects of Harsh Environments
Intubation: Une vision en secours en montagne
17/04/2012
Ibuprofen pour le mal des montagnes
L'utilisation du diamox est reconnu pour la prévention du mal aigu des montagnes (Lire l'article). L'ibuprofen serait également efficace.
Ibuprofen Prevents Altitude Illness: A Randomized Controlled Trial for Prevention of Altitude Illness With Nonsteroidal Anti-inflammatories
Lipman GS et all. doi:10.1016/j.annemergmed.2012.01.019
Study objective
Acute mountain sickness occurs in more than 25% of the tens of millions of people who travel to high altitude each year. Previous studies on chemoprophylaxis with nonsteroidal anti-inflammatory drugs are limited in their ability to determine efficacy. We compare ibuprofen versus placebo in the prevention of acute mountain sickness incidence and severity on ascent from low to high altitude.
Methods
Healthy adult volunteers living at low altitude were randomized to ibuprofen 600 mg or placebo 3 times daily, starting 6 hours before ascent from 1,240 m (4,100 ft) to 3,810 m (12,570 ft) during July and August 2010 in the White Mountains of California. The main outcome measures were acute mountain sickness incidence and severity, measured by the Lake Louise Questionnaire acute mountain sickness score with a diagnosis of ≥ 3 with headache and 1 other symptom.
Results
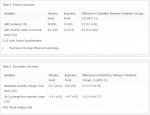
Eighty-six participants completed the study; 44 (51%) received ibuprofen and 42 (49%) placebo. There were no differences in demographic characteristics between the 2 groups. Fewer participants in the ibuprofen group (43%) developed acute mountain sickness compared with those receiving placebo (69%) (odds ratio 0.3, 95% confidence interval 0.1 to 0.8; number needed to treat 3.9, 95% confidence interval 2 to 33). The acute mountain sickness severity was higher in the placebo group (4.4 [SD 2.6]) than individuals receiving ibuprofen (3.2 [SD 2.4]) (mean difference 0.9%; 95% confidence interval 0.3% to 3.0%)
.Conclusion
Compared with placebo, ibuprofen was effective in reducing the incidence of acute mountain sickness.
HEA pas bon en cas de sepsis sévère: Si l'on en croit le "6S trial"
Le choc hémorragique n'est pas le choc septique, mais on peut s'interroger
Background
Hydroxyethyl starch (HES) is widely used for fluid resuscitation in intensive care units (ICUs), but its safety and efficacy have not been established in patients with severe sepsis.
Methods
In this multicenter, parallel-group, blinded trial, we randomly assigned patients with severe sepsis to fluid resuscitation in the ICU with either 6% HES 130/0.42 (Tetraspan) or Ringer’s acetate at a dose of up to 33 ml per kilogram of ideal body weight per day. The primary outcome measure was either death or end-stage kidney failure (dependence on dialysis) at 90 days after randomization.
Results
Of the 804 patients who underwent randomization, 798 were included in the modified intention-to-treat population. The two intervention groups had similar baseline characteristics. At 90 days after randomization, 201 of 398 patients (51%) assigned to HES 130/0.42 had died, as compared with 172 of 400 patients (43%) assigned to Ringer’s acetate (relative risk, 1.17; 95% confidence interval [CI], 1.01 to 1.36; P=0.03); 1 patient in each group had end-stage kidney failure. In the 90-day period, 87 patients (22%) assigned to HES 130/0.42 were treated with renal-replacement therapy versus 65 patients (16%) assigned to Ringer’s acetate (relative risk, 1.35; 95% CI, 1.01 to 1.80; P=0.04), and 38 patients (10%) and 25 patients (6%), respectively, had severe bleeding (relative risk, 1.52; 95% CI, 0.94 to 2.48; P=0.09). The results were supported by multivariate analyses, with adjustment for known risk factors for death or acute kidney injury at baseline.
Conclusions
Patients with severe sepsis assigned to fluid resuscitation with HES 130/0.42 had an increased risk of death at day 90 and were more likely to require renal-replacement therapy, as compared with those receiving Ringer’s acetate.
(Funded by the Danish Research Council and others; 6S ClinicalTrials.gov number, NCT00962156.)
16/04/2012
Techniques de brancardages
Accouchement par voie vaginale
3 Côtés: La valve de Russel
Outre qu'elle présente un dispositif type pansement 3 côtés, cette vidéo est intéressante par la qalité de la présenttaion clinique d'une plaie soufflante.
le thorax se soulève
la fréquence est rapide
la respiration n'est pas harmonieuse
car l'ampliation est faible avec tirage intercostal sans ballotement abdominal
le thorax est ouvert
le thorax souffle
http://www.prometheusmedical.co.uk/uploads/videos/RCS-sim...
FIRST Trial
Resuscitation with hydroxyethyl starch improves renal function and lactate clearance in penetrating trauma in a randomized controlled study: the FIRST trial (Fluids in Resuscitation of Severe Trauma)
James MFM et all. Br. J. Anaesth. (2011) 107 (5):693-702
-------------------------------------
Une étude en faveur des HEA 130/0,4 en ce qui concerne l'atteinte rénale et la production de lactates mais pas en terme de survie, de stabilité tensionnelle et avec une majoration relativement importante des volumes de transfusions dans le groupe HEA. Lire aussi les réactions à cet article
-------------------------------------
Background The role of fluids in trauma resuscitation is controversial. We compared resuscitation with 0.9% saline vs hydroxyethyl starch, HES 130/0.4, in severe trauma with respect to resuscitation, fluid volume, gastrointestinal recovery, renal function, and blood product requirements.
Methods Randomized, controlled, double-blind study of severely injured patients requiring>3 litres of fluid resuscitation. Blunt and penetrating trauma were randomized separately. Patients were followed up for 30 days.
Results A total of 115 patients were randomized; of which, 109 were studied. For patients with penetrating trauma (n=67), the mean (SD) fluid requirements were 5.1 (2.7) litres in the HES group and 7.4 (4.3) litres in the saline group (P<0.001). In blunt trauma (n=42), there was no difference in study fluid requirements, but the HES group required significantly more blood products [packed red blood cell volumes 2943 (1628) vs 1473 (1071) ml, P=0.005] and was more severely injured than the saline group (median injury severity score 29.5 vs 18; P=0.01). Haemodynamic data were similar, but, in the penetrating group, plasma lactate concentrations were lower over the first 4 h (P=0.029) and on day 1 with HES than with saline [2.1 (1.4) vs 3.2 (2.2) mmol litre−1; P=0.017]. There was no difference between any groups in time to recovery of bowel function or mortality. In penetrating trauma, renal injury occurred more frequently in the saline group than the HES group (16% vs 0%; P=0.018). In penetrating trauma, maximum sequential organ function scores were lower with HES than with saline (median 2.4 vs 4.5, P=0.012). No differences were seen in safety measures in the blunt trauma patients.
Conclusions In penetrating trauma, HES provided significantly better lactate clearance and less renal injury than saline. No firm conclusions could be drawn for blunt trauma.
-------------------------------------
15/04/2012
Battle mind training: Le système
| Tags : ptsd, psychiatrie