20/03/2016
Blessés par balle: Civil et guerre, différent !
12/03/2016
Douleur: Pendant l'évacuation, Kétamine = Morphine ?
Prehospital Pain Medication Use by U.S. Forces in Afghanistan
Shackelford SA et Al. Mil Med. 2015 Mar;180(3):304-9
We report the results of a process improvement initiative to examine the current use and safety of prehospital pain medications by U.S. Forces in Afghanistan. Prehospital pain medication data were prospectively collected on 309 casualties evacuated from point of injury (POI) to surgical hospitals from October 2012 to March 2013. Vital signs obtained from POI and flight medics and on arrival to surgical hospitals were compared using one-way analysis of variance test. 119 casualties (39%) received pain medication during POI care and 283 (92%) received pain medication during tactical evacuation (TACEVAC). Morphine and oral transmucosal fentanyl citrate were the most commonly used pain medications during POI care, whereas ketamine and fentanyl predominated during TACEVAC.

Ketamine was associated with increase in systolic blood pressure compared to morphine (+7 ± 17 versus −3 ± 14 mm Hg, p = 0.04). There was no difference in vital signs on arrival to the hospital between casualties who received no pain medication, morphine, fentanyl, or ketamine during TACEVAC. In this convenience sample, fentanyl and ketamine were as safe as morphine for prehospital use within the dose ranges administered. Future efforts to improve battlefield pain control should focus on improved delivery of pain control at POI and the role of combination therapies.
| Tags : kétamine
Douleur: Kétamine d'abord ?
Prehospital and En Route Analgesic Use in the Combat Setting: A Prospectively Designed, Multicenter, Observational Study
Lawrence N. Petz LN et Al. , Mil Med. 2015 Mar;180(3 Suppl):14-8
Background:
Combat injuries result in acute, severe pain. Early use of analgesia after injury is known to be beneficial. Studies on prehospital analgesia in combat are limited and no prospectively designed study has reported the use of analgesics in the prehospital and en route care setting. Our objective was to describe the current use of prehospital analgesia in the combat setting.
Methods:
This prospectively designed, multicenter, observational, prehospital combat study was undertaken at medical treatment facilities (MTF) in Afghanistan between October 2012 and September 2013. It formed part of a larger study aimed at describing the use of lifesaving interventions in combat. On arrival at the MTF, trained on-site investigators enrolled eligible patients and completed standardized data capture forms, which included the name, dose, and route of administration of all prehospital analgesics, and the type of provider who administered the drug. Physiological data were retrospectively ascribed as soon as practicable. The study was prospectively approved by the Brooke Army Medical Center institutional review board.
Results:
Data were collected on 228 patients, with 305 analgesia administrations recorded. The predominant mechanism of injury was blast (50%), followed by penetrating (41%), and blunt (9%). The most common analgesic used was ketamine, followed by morphine.

A combination of analgesics was given to 29% of patients; the most common combination was ketamine and morphine. Intravenous delivery was the most commonly used route (55%). Patients transported by the UK Medical Emergency Response Team (MERT) or U.S. Air Medical Evacuation (Dust-off) team were more likely to receive ketamine than those evacuated by U.S. Pararescue Jumpers (Pedro). Patients transported by Medical Emergency Response Team or Pedro were more likely to receive more than 1 drug. Patients who received only ketamine had a higher pulse rate ( p < 0.005) and lower systolic blood pressure ( p = 0.01) than other groups, and patients that received hydromorphone had a lower respiratory rate ( p = 0.04).
Conclusions: In our prospectively designed, multicenter, observational, prehospital combat study, ketamine was the most commonly used analgesic drug. The most frequently observed combination of drugs was ketamine and morphine. The intravenous route was used for 55% of drug administrations.
| Tags : kétamine
08/03/2016
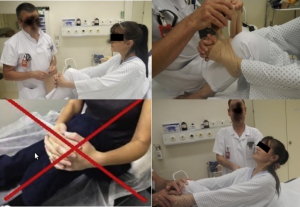
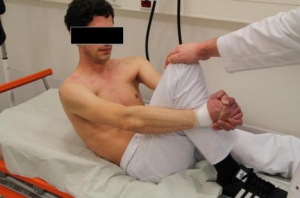
Epaule luxée ! Réduire seul
Simple self-reduction method for anterior shoulder dislocation
Reiner Wirbel et al. Journal of Acute Disease (2014)207-210
C'est la plus fréquente des luxations. La diversité des méthodes de réduction illustre bien la difficulté qu'il peut y avoir à la réduire sans avoir recours à une anesthésie/sédation. C'est encore plus vrai en cas d'isolement extrême. Une méthode à connaître.