25/03/2026
Arctic Military Conference on Cold Weather Medicine
21/03/2026
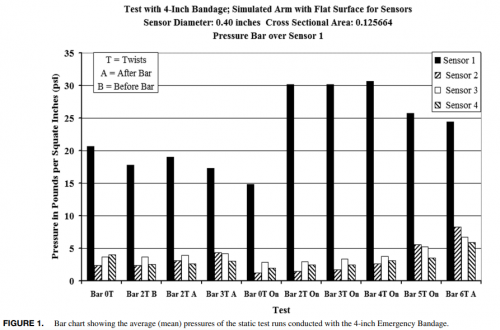
Pansement Israélein: Interrêt de la barre de compression locale
17/03/2026
Délais de prise en charge allongés et pansement hémostatique: Danger

03/03/2026
Intubation difficle: Pas qu'anatomique
Managing the Physiologically Difficult Airway in Critically Ill Adults
Jabaley CS. Crit Care. 2023 Mar 21;27(1):91. doi: 10.1186/s13054-023-04371-3.
Un document très intéressant qui présente de manière très claire les enjeux de l'intubation difficile qui n'est pas qu'anatomique.
|
Risks and risk prediction |
|
Cardiovascular instability, hypoxemia, and cardiac arrest are the most common adverse events associated with tracheal intubation |
|
Risk factors for cardiovascular collapse include age, shock, hypoxemia, advanced critical illness, and propofol administration |
|
Hemodynamic optimization |
|
Etomidate and ketamine may impact hemodynamics less than propofol |
|
A crystalloid bolus prior to intubation has not been associated with improved hemodynamics, even in patients receiving positive pressure ventilation |
|
Given the frequency of cardiovascular instability, vasopressors should be readied as part of preparation for tracheal intubation |
|
Mitigating hypoxemia |
|
Standard pre-oxygenation strategies are inadequate to safely extend the apneic interval in patients with moderate to severe respiratory failure |
|
Non-invasive ventilation can be used with or without high flow nasal oxygen and is more effective than high flow nasal oxygen alone |
|
While historically avoided, bag-mask ventilation improves oxygenation during airway management and can be employed either preemptively or for rescue |
|
First pass success |
|
Multiple attempts at intubation increase the risk of adverse events |
|
Depending on the preferences and expertise of the intubating clinician, video laryngoscopy or direct laryngoscopy with adjuncts may improve first pass success |
|
Checklists improve adherence to complex, multi-step processes and may help prompt preparation for physiologic trespass |
01/03/2026
Trauma: Exsufflation à l'aiguille. Pas sûr du tout

